|
9/10/2023 0 Comments Closed fracture of sacrum 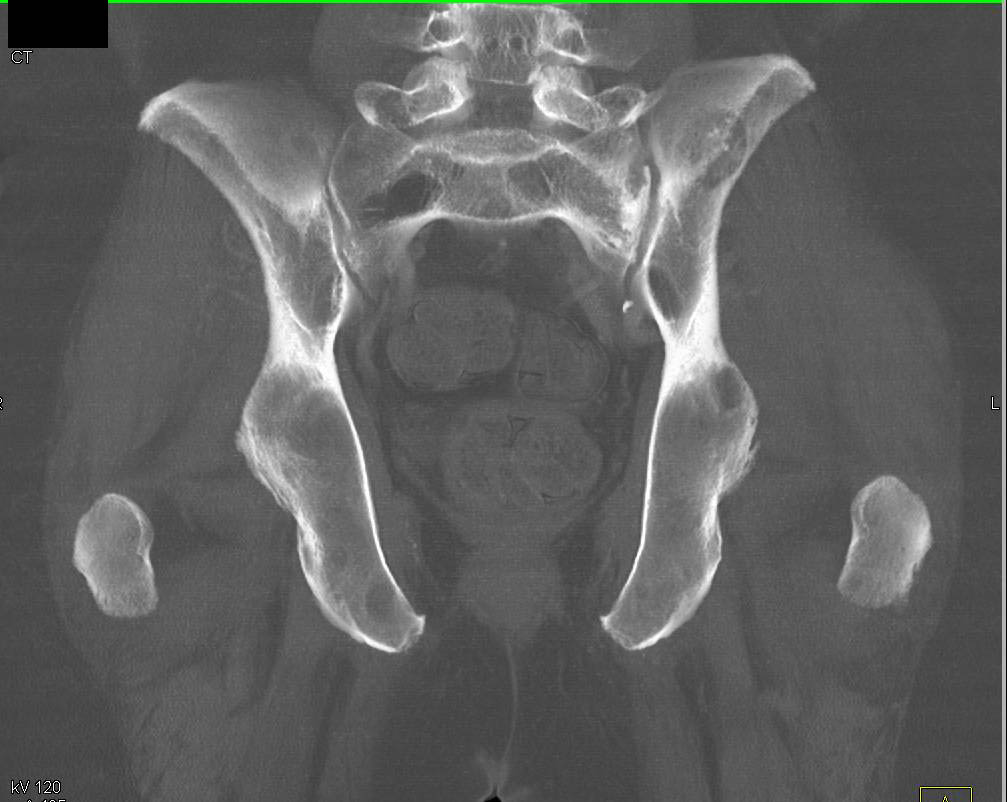
Pelvic examination revealed a positive FABER (flexion, abduction and external rotation test). She had undergone resection and chemotherapy for colonic carcinoma five years earlier, and had sustained a Colles’ fracture. Case 2.Ī 73-year-old woman with a painful gait due to left-sided sacral pain presented eight weeks after a trivial domestic fall. 
There is sclerosis at the left and right sacral alae indicating healthy process. b) Axial CT scan demonstrates bilateral sacroiliac joint screws in place. Because of her chronic disability and relatively good bone quality on MRI and CT she underwent bilateral sacroiliac screw fixation.Ĭase 1 – a) Post-operative radiograph demonstrating bilateral sacroiliac screws and consolidation of the pubic rami fractures. Magnetic resonance imaging showed changes in both alae confirming bilateral sacral insufficiency fractures ( Fig. A CT scan showed sclerosis of the right alar wing, indicating an attempt at healing ( Fig. A bone scan ( 99mTc medronate methylene diphosphonate) demonstrated the ‘H’ sign, indicating bilateral activity at the sacral alae ( Fig. An anteroposterior (AP) radiograph of the pelvis revealed fractures of the right superior and inferior pubic rami ( Fig. The levels of alkaline phosphatase were raised (309 IU/l, 70 to 300 IU/l), but her biochemical profile and inflammatory markers (C-reactive protein, white cell count, erythrocyte sedimentation rate) were normal. On examination, she had an antalgic gait and localised tenderness over her sacroiliac joints, but no neurological deficit. After eight weeks, she noted that the sacral pain was bilateral. Her pain was felt over the right sacroiliac joint and at the pubic symphysis. She did not seek medical attention initially. Case reports Case 1.Ī 56-year-old woman with osteoporosis was referred with a five-month history of continuing low back and pelvic pain after a low-impact fall at home. We present our experience of percutaneous sacroiliac screw fixation for the treatment of such fractures in three patients. Interventional methods of treating sacral insufficiency fractures have been described, 4, 6 based on injection of polymethylmethacrylate (PMMA) cement into the fracture site to reduce painful micromovement and allow earlier rehabilitation. 4 The subsequent complications are well recognised and interfere further with recovery. 3 These measures often fail to provide adequate pain relief, with consequent prolonged bed rest. 2 They are invariably treated non-operatively with bed rest, analgesia and early rehabilitation. 
1 Sacral insufficiency fractures are often overlooked as a potential cause of low back and pelvic pain in patients presenting without a significant history of trauma, thereby resulting in diagnostic delay. This article reviews the approach to sacral fracture diagnosis and management.Osteoporotic fractures of the pelvis are more prevalent than is widely appreciated and are increasing in incidence. Surgical fixation techniques include percutaneously placed iliosacral screws, posterior sacral "tension band" fixation, and for certain fracture patterns osteosynthesis that incorporates the lower lumbar spine (lumbopelvic or triangular fixation). Stable nondisplaced fractures are usually treated nonoperatively, while significantly displaced fractures require reduction and internal fixation. Once identified, correct classification of a sacral fracture can facilitate ideal treatment strategies. While displaced fractures can be easily diagnosed on high quality plain radiographs, nondisplaced or transverse fracture patterns may be difficult to diagnose without a computed tomography scan. An understanding of the anatomic relation of the sacrum to the lumbar spine, pelvis, and surrounding neurovascular structures is critical in evaluating functional deficits that may be associated with sacral fractures. Sacral fractures are commonly associated with pelvic ring fractures due to high-energy mechanisms of injury. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |

 RSS Feed
RSS Feed
